If people — particularly elderly people — don't want doctors to take extreme measures to potentially save their lives, does that increase Vermont's COVID-19 death rate?
Note: Our show is made for the ear. As always, we recommend listening if you can!
Sometimes a question about one thing becomes, well, a question about something else. That's what happened for Melanie Peyser, our latest winning question-asker. Melanie originally submitted this question, and our audience selected it in a public voting round:
Public data suggests Vermont’s COVID-19 death rate (deaths/confirmed cases) is high compared to other states. What’s the story?
Brave Little State is VPR’s people-powered journalism project. We answer questions about Vermont that have been submitted and voted on by our audience, because we believe our journalism is better when you're a part of it.
Subscribe to Brave Little State for free, so you never miss an episode:
Loading...
Peyser lives in Addison County and works in international development. She has an eye for data. So as the coronavirus begins affecting Vermonters, she starts spending a lot of time looking at data online.
“You know, this is sort of amateur sleuthing,” she says. “And early on, I started to become alarmed that it seemed like we had a particularly high death rate compared to our known number of cases.”
And then, she hears about something Vermont’s Commissioner of Health, Mark Levine, said when he spoke about the state’s death rate during a press conference. This was in late March, when Vermont’sfirst nursing home outbreak was underway.
“For many in that population, the goals of care — due to other conditions that were sometimes cardiac, sometimes dementia, et cetera — the goals of care were not aggressive treatment in a hospital or ICU setting," Levine said.
Because many of these nursing home residents had other serious conditions, Levine said they had already told their doctors not to take extreme measures to try to save their lives. These "goals of care" are often documented in what’s called an advanced directive.
And at that press conference, Levine said only one of Burlington Health & Rehab’s then-seven COVID-19 deaths had occurred at a hospital.
“So I think that makes our numbers look worse,” Levine said.
Loading...
And that’s what got Peyser thinking: “Is that the reason that we have such a high rate?”
By the time Melanie Peyser and I chatted, the death rates of a dozen or so other states had actually surpassed ours. It was clear what Peyser was really interested in was what Levine had said about advanced directives – those documents and conversations people have about what kind of interventions they do and don’t want at the end of their lives.
Here’s the question she asked me to answer:
I am wondering how advanced health care directives are affecting treatment and outcomes for COVID-19 patients in Vermont.
Digging into the data
Back in late March, Vermont’s case fatality rate – or deaths per COVID patient – did stand out.
Take March 27, the day Commissioner Levine made the comments about advanced directives. That day, Vermont had the highest death rate in the country: more than 5% of Vermont’s known COVID-19 patients had died. In Maine and New Hampshire, fewer than 1% of COVID patients had passed away.
“Initially that is high, because of the outbreaks in long-term care facilities and other vulnerable populations,” says Jessie Hammond, the public health statistics manager at the Vermont Department of Health.
On mobile? Click here to see the infographic.
Hammond says it’s not just that COVID-19 spreads fast in places like care facilities.
“You know, they're in a care facility because of their health, which would put them at a greater risk for death,” she says.
Since late March, Vermont’s case fatality rate has remained steady, while other states' rates, including our neighbors', have gone up. Now our death rate ranks 14th of the 50 states.
And of course lots of factors affect this number. If the disease only occurs nursing homes, the number will be really high. If it spreads in younger, healthier populations, the death rate will go down. Widespread testing also influences the death rate.
Our question-asker Melanie Peyser wants to know if end-of-life planning is leading patients to forgo potentially life-saving interventions, bumping up the death rate as a result.
At Birchwood Terrace
It was Thursday, April 2 when University of Vermont Medical Center head of palliative medicine Bob Gramling got a call from the head of geriatrics. Birchwood Terrace, a 144-bed skilled nursing facility in Burlington, was on the brink of a major outbreak. The doctor told Gramling that there were patients with symptoms of COVID-19 across the facility.
Gramling recalls him saying:
“ … You know, ‘This could this could grow fast, and if so, we might need your help to be on the ground with us to take care of these people.’”
In a place like Birchwood, Gramling knew how quickly this disease can take lives and sideline staff. So he started calling colleagues.
Four days later, a spiritual health worker, five palliative care specialists and eight RNs from UVMMC began their deployment to Birchwood.
More than anything else, they were there to have conversations with patients and their families. The specialists asked the Birchwood residents: If you got COVID-19, and it got bad, would you want to go to the hospital — even if interventions there might not help?
“I don't know of other places in the country that have done this,” Gramling says. “It is quite possible it has happened. But, yes, it is a rare event, if not a unique event.”
The team even had an RV on campus. Two members were there 24/7.

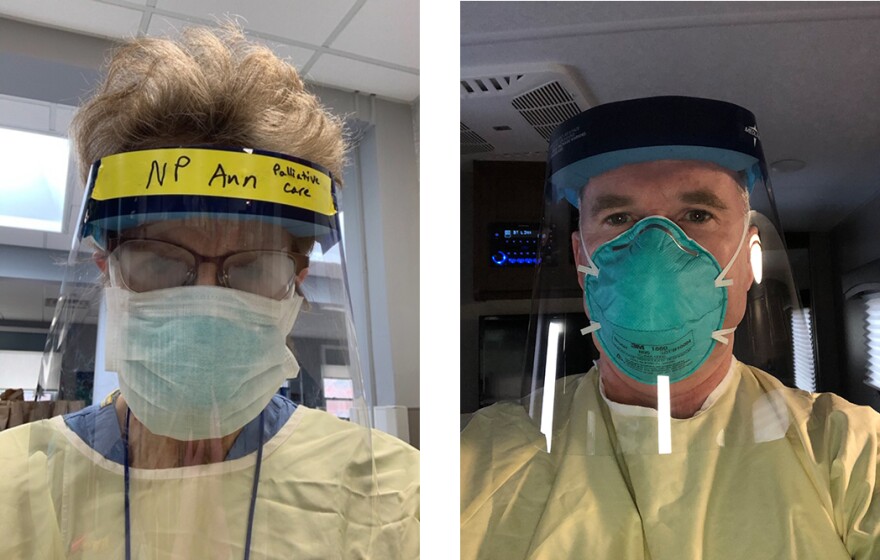
Ann Laramee is one of the nurse practitioners on the team that deployed to Birchwood.
“And you know, we do these conversations all the time, multiple times every day, but this is different,” she says. “There’s an urgency and an intensity to this, knowing that things could change very fast.”
Laramee, who tends to answer questions with anecdotes, says on her first day at Birchwood, she met a gentleman who had tested positive for COVID-19 but didn’t have any symptoms.
“He was a delightful guy, really loved by the staff there,” she says. “He liked to play trivia. He called his siblings every single day.”
That first day, Laramee got to know his advanced directive. It clearly stated that he did not want to be resuscitated or intubated. But, she knew, there were other things the hospital could do that might be helpful. So, she got to know him. She learned that he considered Birchwood a home. And the thing he lived for most? His daily phone calls with his siblings.
Part of advanced planning is getting to know these things: What does someone live for, and what constitutes suffering – for them?
A couple days later, the man’s oxygen saturation dropped. Even though he still felt fine, he was now at risk of sudden respiratory failure. They put him on oxygen at the nursing home, but Laramee needed to know if they should bring him to the hospital.
“I sat down and said I needed to talk to him about something serious,” she says.
She told him again how fast symptoms could come on, and that people were dying. She asked him: Would he want to go to the hospital, knowing he might die there?
Laramee says he thought quietly for a long time.
“He basically was a not-answer, but he wasn’t saying he wanted to go to the hospital,” she says.
The next day, she went back to speak with him. Again, he was needing oxygen, but not feeling any symptoms.
“I asked him again about our conversation yesterday. You know, ‘How did that feel?’ And he sat again for a long time just looking and thinking,” she says. “And he said, ‘You're not going to make me go to the hospital, are you?’”
Laramee says she did her best to make sure they understood each other. This disease can take a quick turn for the worse, and there was a small chance that being at the hospital could extend his life. But it was also likely if he went, he could die there, away from the caretakers he knows and loves.
That evening, she says the man video chatted with his siblings for hours. They were still going at 7 p.m., when she went home.
“They were still talking, they were sharing photos,” Laramee says. “And that night, his symptoms rapidly changed. And by the time I got there in the morning, he had actually died. It happened that quickly.”
Loading...
On choosing how to die
All of the 28 COVID-positive and presumed positive patients who got seriously ill at Birchwood decided to stay there, and not to go to the hospital. Twenty passed away at the nursing home. Eight survived.
What was remarkable about the palliative care team’s arrival was that it allowed patients and families to discuss the disease and their preferences early – before residents had symptoms or needed urgent care.
At another nursing home – Burlington Health and Rehab, which had the first outbreak – 11 patients died after getting COVID-19. Only three chose to go to the hospital. A spokesperson for that facility says the center’s providers discuss all patients’ end-of-life care with them every three months, and did so during the outbreak as well.
Loading...
As for whether patients’ decisions are affecting Vermont’s death rate — like Health Commissioner Mark Levine suggested early on — is still unclear.
“The default in our health care system is to do everything," Laramee says. "I suppose that, you know, if we're asking people and giving having them participate in decision-making, they're going to choose a path that maybe they wouldn't have if they weren't asked – maybe."
She adds: “You know, there's no treatment to COVID. So, the people that are surviving after being intubated, I don't know what the stats are, but it's not very many. So in many ways, we don't have a choice: Their body’s going to do what it's going to do.”

Thanks to Melanie Peyser for the great question, and to Dr. Katie Auriemma at the Hospital of the University of Pennsylvania.
Brave Little State is a production of Vermont Public Radio. We have support from the VPR Innovation Fund, and from VPR’s sustaining members. You can support us at bravelittlestate.org/donate. We’re also on Instagram and Twitter @bravestatevt. You can also sign up for our occasional newsletter.
This episode was produced by Emily Corwin, with editing from Mark Davis. Brave Little State’s host and creator is Angela Evancie, and our digital producer is Elodie Reed. We have engineering support from John Billingsley. Ty Gibbons composed our theme music, and other music is by Blue Dot Sessions.





